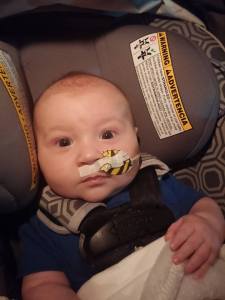
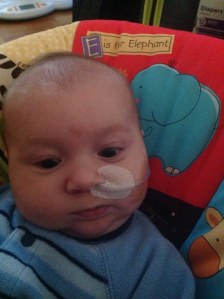
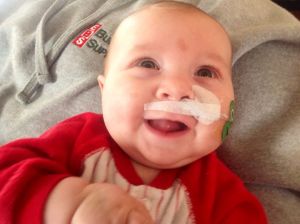
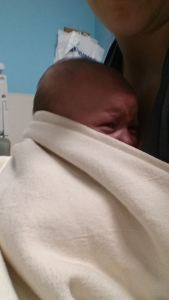
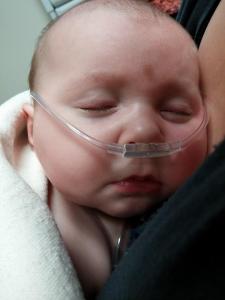
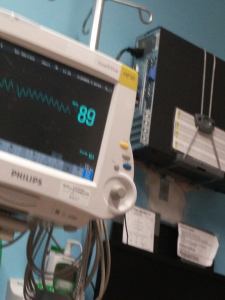
Upon arriving at Maine Med Sunday afternoon, we were taken straight to a room in the Barbara Bush children’s Hospital (BBCH). After asking a million questions about what brought us here, the admitting doctors made the decision to stop letting Isaac eat by mouth and feed him via an NG tube (a tube that goes into his nose and straight into his stomach, bypassing his airway junction).
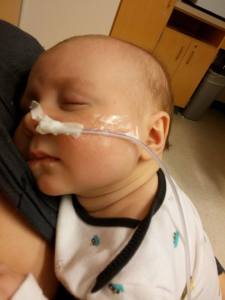
Within a day or two after he received the NG tube, his wheezing stopped and his lungs cleared. I was blown away by how quickly his breathing improved. He hadn’t sounded that good in months! The plan was to continue tube feeding him until the pulmonologist and ENT could coordinate a bronchoscopy in the OR, using two types of cameras. Unfortunately this couldn’t be arranged until Thursday, so we were basically just waiting around until then.
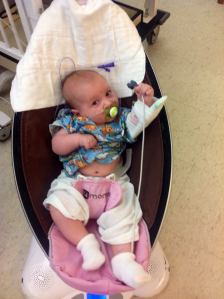
One of the hospital ENT doctors stopped by with a bedside camera that he inserted into Isaac’s nose so he could visualize his throat and vocal cords. He found swelling, redness, and irritation which suggested that Isaac was suffering with GERD. I had been trying to treat this with reflux medications in the weeks prior to being admitted to the hospital but I was having a very hard time getting him to take the medication without choking and aspirating and vomiting. One benefit to now having the feeding tube is that it can also be used to give him medications without worrying about Isaac struggling with them.
On Thursday, Isaac was taken to the operating room and once again, I had to leave my baby in the hands of surgeons. They let me hold him as they put him under. He stiffened and twitched a little and then his eyes rolled back and he was out. Waiting has always been the hardest part. Finally, the pulmonologist came out to discuss his findings with us. Isaac didn’t have any anatomical defects but he did have copious bubbly secretions coating his trachea and lungs. The pulmonologist explained this could be due to A) Cystic Fibrosis (which he doubted because at this age, he had never seen it present in such a way. Regardless, he recommended a sweat test to rule it out, especially since I am a carrier), B) Infection (which he also doubted because Isaac hasn’t had any other signs of an infection and it has been going on for so long), or C) Aspiration. He was leaning towards C, which confirmed my concerns I’ve been trying to convey for so long.
The following day, a swallow study was ordered. This showed some delay with swallowing and penetration (putting him at increased risk for aspiration) but again showed no actual aspiration. Not surprising to me because for that whole 3 minutes, he didn’t have any choking. The problem with these kinds of tests are that they only give you a brief glance at that moment in time. And because his choking wasn’t occurring 100% of the time, it makes sense they didn’t find anything with that test.
We had the sweat test to check for cystic fibrosis completed while we were still inpatient. (Our first was also tested for this, due to the amount of mucus he was passing in his diapers.) We had to place little sweat collector discs on both of his legs, crank the heat in his room, and bundle him for 30 minutes.
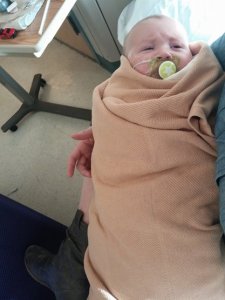
The sweat was collected into the discs that contained a blue dye so we could visualize the amount. Isaac’s results were normal.
Moving forward from there, the doctors wanted to try and see how he tolerated thickened milk from a bottle. I had two options, neither of which I wanted: thicken my breast milk with rice cereal, or switch to formula which could be thickened with powder. At this point I felt like I had to choose between his lungs and his gut. I decided that breast milk thickened with rice cereal would be less of a shock to his system than switching completely to formula. We started with one ounce thickened with one teaspoon and then the rest through his tube. This seemed to make his reflux worse so the following day we tried one ounce to two teaspoons. Most of the time, he tolerated this without choking but as we began to increase the amount, he began to struggle again.
The GI doctor who was on that weekend was not very willing to listen to me or offer a plan of action other than just persevering with the thickened feeds. Monday, the GI doctor on is actually the one we’ve been working with for Joseph. We’ve known her for years and she was familiar with our family too. The rappor was already there; I knew she would listen to me and I trusted her judgement. She was willing to view the videos I had taken of Isaac’s choking and breathing. She wanted to order one more test and if it came back normal, would discuss sending us home with the feeding tube. The test was an esophagram to look more specifically for a fistual connecting his trachea and esophagus. This test was negative, so we were finally about to discuss being discharged and sent home. The only explanation they could come up with for Isaac’s feeding difficulties was an immature feeding reflex and GERD that he would hopefully outgrow. In the meantime, we would have the tube to help feed him so he wouldn’t be at high risk for developing respiratory distress secondary to aspiration again. I have to say I was frustrated and relieved at the same time. This is not something I ever wanted for my child and at the same time, I wasn’t so scared to feed him anymore because I had the tube as an alternative. The plan we came up with was to try each feed by mouth first and if there was any struggle, stop and finish with the tube. This way, he would continue to have opportunities to eat by mouth and not become completely dependent on the tube and forget how to eat (a very real concern for tube-fed babies).
Tuesday came and we were finally able to go home! I discussed with our GI doctor my thoughts on discontinuing to thicken his feeds and resuming breastfeeding; the thickened milk didn’t seem to be making enough of a difference for me to want to continue with it. The way I see things, if he’s going to choke regardless, I’d rather he choke on just breast milk than milk with rice cereal in it. That would be the lesser of two evils from the standpoint of his lungs. I had read once that if you are going to choke on anything, breast milk is what you want because of its antibacterial properties. I was given the OK to try out different feeding techniques and see what actually makes a difference and what works for him.
Discharge from the hospital was a nightmare! There was a breakdown in the communication between the hospital, the infusion supply company, and the home nursing company. Eventually everything was resolved but I was pulling my hair out for a little while there! We were rushed out thinking we had to be home to meet the home nurse by noon. The infusion supplies were supposed to be sent to the hospital so we could bring them home with us but nothing had arrived by the time we left. And on the way home, I got a call from the home nurse asking if I wanted to set up a time to meet her…I wasn’t confident in changing the NG tube (I’ve seen it done and in nursing school I’d practiced on mannequins but I’ve never actually placed one on a person, let alone my baby) and no one went over the expectations for how often to change it. Despite the confusion, we were just so glad to be going home!